Hip osteoarthritis is a common condition that commonly affects people as they age. It occurs when the protective cartilage on the ends of bones wears down over time.
This joint disorder can result in pain, stiffness and reduced mobility of the hip. Although it is more common in older adults, it can also affect younger individuals due to injury or genetic factors. Understanding this condition is crucial for managing symptoms effectively and maintaining an active lifestyle.
Contents
ToggleCauses of Hip Osteoarthritis
Hip osteoarthritis is a condition that impacts many people, especially as they grow older. Understanding the causes can be incredibly helpful in managing and possibly slowing the progression of the condition. We explore the main causes, which range from ageing to lifestyle choices.
Age-Related Factors
Hip osteoarthritis is sometimes referred to as a “wear-and-tear” disease, primarily because age is one of the biggest factors. As we age, the cartilage that acts as a cushion between bones in our joints begins to wear and break down. This degeneration reduces the shock-absorbing capabilities of the cartilage, leading to pain and reduced movement. The longer we have been using our joints, the more likely they are to have experienced some wear and tear. This explains why hip osteoarthritis tends to appear or worsen as people get older.
As we age, the body’s natural ability to resist cartilage damage diminishes. This means any minor injuries or strains may have lasting effects, further contributing to the development of osteoarthritis.
Genetic Predisposition
Some people find themselves battling hip osteoarthritis no matter how gentle they have been on their joints throughout their lives. Genetics can play a significant role in this. If you have a family history of osteoarthritis, there may be a higher chance that you will develop it too.
Certain genetic markers are linked to an increased risk of developing osteoarthritis, meaning that some individuals are more prone to the condition due to their genetic makeup. Although we can’t alter our genetic predisposition, being aware of it can guide us in taking proactive steps to manage our joint health.
In addition, some of us are born with abnormal hip anatomy, which can pre-dispose to premature osteoarthritis. Hip dysplasia and congenital dislocation of the hip are examples of such conditions.
Lifestyle and Environmental Influences
While genetics and age are beyond our control, lifestyle choices significantly influence the development of hip osteoarthritis. Obesity, for one, is a major risk factor. Carrying extra weight puts additional stress on hip joints, accelerating the degradation of cartilage.
Physical activity is another piece of the puzzle. People with physically demanding jobs or those who engage in high-impact sports are more likely to develop osteoarthritis due to the repeated stress on their joints. However, it’s not all bad news. Frequent but moderate exercise can help maintain joint health by keeping the muscles around the joints strong and supportive.
Environmental factors can also be contributors. Consider previous injuries like fractures, dislocations or joint surgery may have damaged the joint surface cartilage or altered the stability of the joint, which can lead to osteoarthritis over time.
Symptoms of Hip Osteoarthritis
Recognising the symptoms of hip osteoarthritis early can make a world of difference in managing the condition effectively. Let’s take a closer look at what to watch for, from that initial morning stiffness to more noticeable discomfort and limitations.
Pain and Stiffness
One of the classic signs of hip osteoarthritis is joint pain. This pain generally starts as a dull ache and can progressively worsen over time. Many people find this discomfort is often more noticeable after periods of inactivity, such as first thing in the morning or after sitting for a long time. Pain is typically felt in the groin, and thigh. It can also be felt in the buttock and may radiate into the knee. It is also common for the pain to intensify after physical activity or at the end of the day. Morning stiffness usually eases up as you move around, but the relief may not be long-lived
Reduced Range of Motion
If you are having difficulties in your everyday movements, hip osteoarthritis might be to blame. You may notice that it is harder to perform activities that require turning or pivoting. Simple motions like walking, bending or even putting on socks and shoes become challenging due to a reduced range of motion.
Over time, individuals with hip osteoarthritis often experience decreased mobility and loss of walking distance, making it important to seek treatment and employ exercises that help maintain joint flexibility and muscle strength. Avoiding movement due to discomfort can lead to further stiffness in the joint, creating a vicious cycle of reduced activity and increased pain.
Swelling and Tenderness
Being a deep seated joint, visible swelling around the hip is uncommon. Swelling is the body’s response to inflammation within the joint and can occasionally result in visible puffiness around the hip. Alongside swelling, tenderness in the hip area is another symptom that often crops up, especially when pressing on or near the affected joint.
This tenderness or inflammation might make sitting for long periods uncomfortable and could also lead to limping or changes in the way one walks. Paying attention to such changes is crucial as they can significantly impact your overall quality of life.
Understanding these causes and symptoms my help you to take control of the problem, encouraging you to seek early intervention, proper treatment and lifestyle adjustments to manage hip osteoarthritis effectively.
Treatments for Hip Osteoarthritis
Understanding the various treatment options for hip osteoarthritis can help manage symptoms, alleviate pain and maintain mobility. There is no one-size-fits-all approach, so it is key to explore what works best for you.
The different treatments available for hip osteoarthritis are:
Pain Management Techniques
Pain management is often the first line of defence against hip osteoarthritis. Here are some common techniques:
– Medications: Over-the-counter pain relievers such as paracetamol or ibuprofen can be helpful. In some cases, your doctor might prescribe stronger medications to provide relief.
– Topical Treatments: Creams and gels containing anti-inflammatory agents can be applied directly to the hip area to alleviate pain.
– Heat and Cold Therapy: Applying a warm compress or heating pad can relax muscles and ease discomfort. Cold packs can help reduce inflammation and numb the area temporarily.
– Diet and Supplements: Consuming a diet rich in omega-3 fatty acids and antioxidants may support joint health. Some people find supplements like glucosamine and chondroitin helpful, though it is best to discuss these with a healthcare provider first.
– Injections: XR-guided steroid injections can be helpful in providing relief from arthritic hip pain.
Physiotherapy and Exercise
Physiotherapy plays a vital role in managing hip osteoarthritis and regular exercise is crucial for maintaining joint function and mobility.
– Tailored Exercise Programmes: A physiotherapist can design a personalised exercise plan that strengthens the muscles around your hip, improving stability and flexibility. Exercises might include low-impact activities like swimming, cycling or yoga.
– Range of Motion Exercises: These help maintain mobility in the hip joint and reduce stiffness, making everyday activities easier and less painful.
– Strength Training: Building muscle strength, especially in the pelvic and thigh regions, can take some of the pressure off the hip joint, aiding in pain reduction.
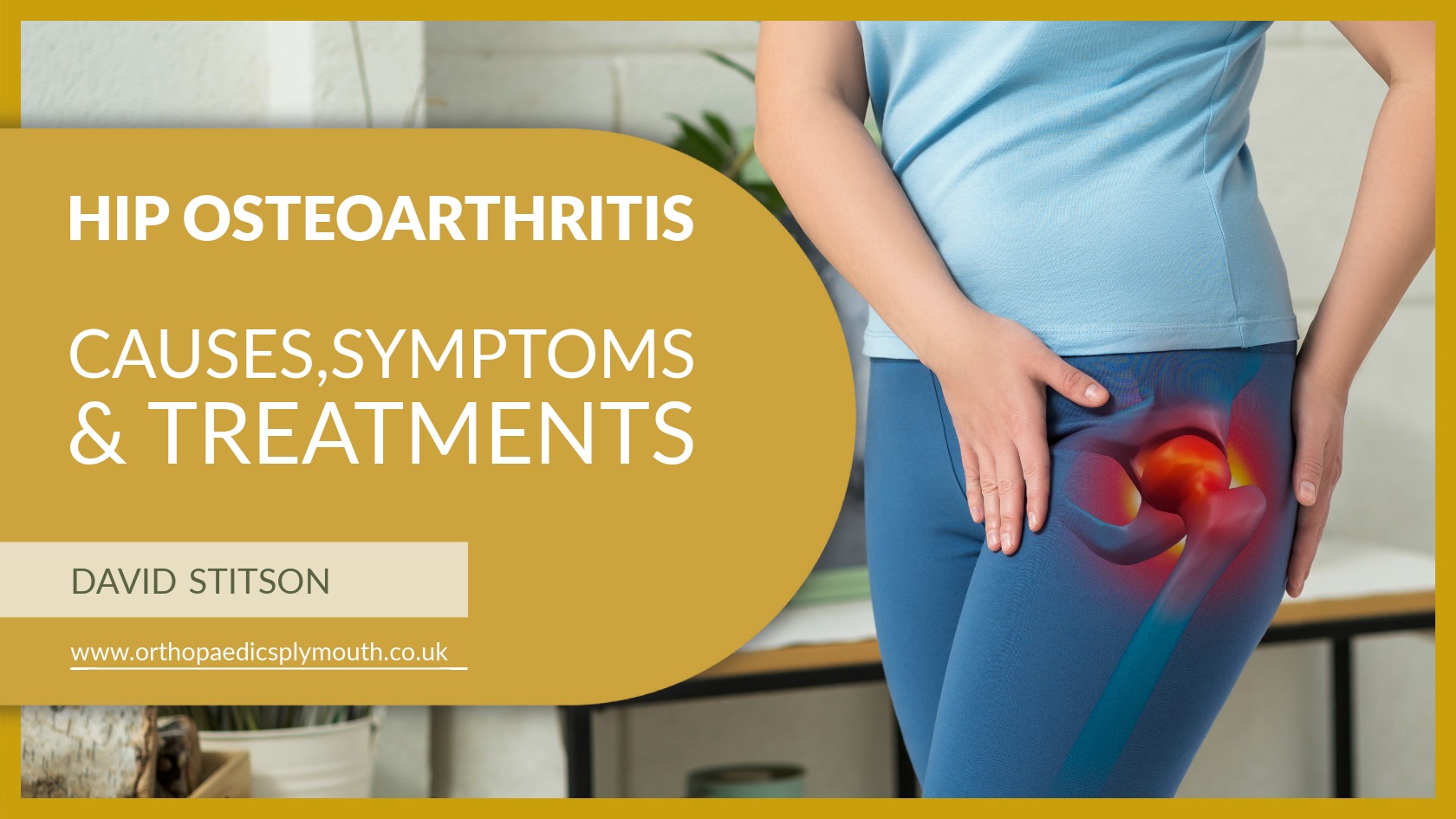
Surgical Options
When other treatments are ineffective, and pain and mobility worsen, surgical options may be considered.
– Arthroscopy: This minimally invasive surgery involves smoothing out rough cartilage and removing any loose pieces. It is occasionally recommended for milder cases of hip osteoarthritis if associated with hip dysplasia.
– Hip Resurfacing: Indicated for some younger, more active patients, this procedure reshapes and caps the joint surfaces with metal.
– Total Hip Replacement: If pain is severe and hindering your quality of life, a total hip replacement might be the answer. In this procedure, the damaged joint is replaced with a prosthetic one, offering a new lease on life for many.
These treatments offer hope in managing hip osteoarthritis, ensuring a better quality of life through effective pain relief and improved mobility. Remember, it is important to consult with healthcare professionals to determine the best plan for your specific needs.
Get Orthopaedic Surgery in Plymouth in just 4-6 weeks
⇒ Consultation in 7 days or less
⇒ Consultation to surgery, 4-6 weeks
Hip Osteoarthritis FAQs
Q: What is hip osteoarthritis?
A: Hip osteoarthritis is a chronic joint condition where the cartilage that cushions the hip joint breaks down and wears out over time, leading to pain and stiffness.
Q: Who is at risk for developing hip osteoarthritis?
A: Risk factors include age, genetics, previous joint injuries, obesity and repetitive stress on the hip joint from certain sports or occupations.
Q: Can lifestyle changes help manage hip osteoarthritis?
A: Absolutely! Maintaining a healthy weight, engaging in low-impact exercises like swimming or cycling and following a balanced diet rich in anti-inflammatory foods can significantly help in managing the symptoms.
Q: Are there surgical options for treating hip osteoarthritis?
A: Yes, in severe cases, surgical options, such as total hip replacement, might be recommended by your doctor to relieve pain and restore mobility. Always discuss with your healthcare professional to determine the best course of action for you.




![Am I Ready for a Knee Replacement? [Free Checklist] | Mr David Stitson | CONSULTANT ORTHOPAEDIC SURGEON | Plymouth Am I Ready For A Knee Replacement? | David Stitson, Consultant Orthopaedic Surgeon in Plymouth.](https://orthopaedicsplymouth.co.uk/wp-content/uploads/2026/05/DJS-Blog-1-Am-I-Ready-For-A-Knee-Replacement--150x150.jpeg)